What Is Adenoid Hyperplasia? A Complete Guide
If your child snores loudly at night, breathes through their mouth constantly, or keeps getting ear infections — adenoid hyperplasia might be the reason. It’s one of those conditions that often goes unnoticed until the symptoms pile up. Understanding what it is, why it happens, and what you can do about it can save a lot of frustration for both parents and kids.
What Is Adenoid Hyperplasia and Why Does It Happen?
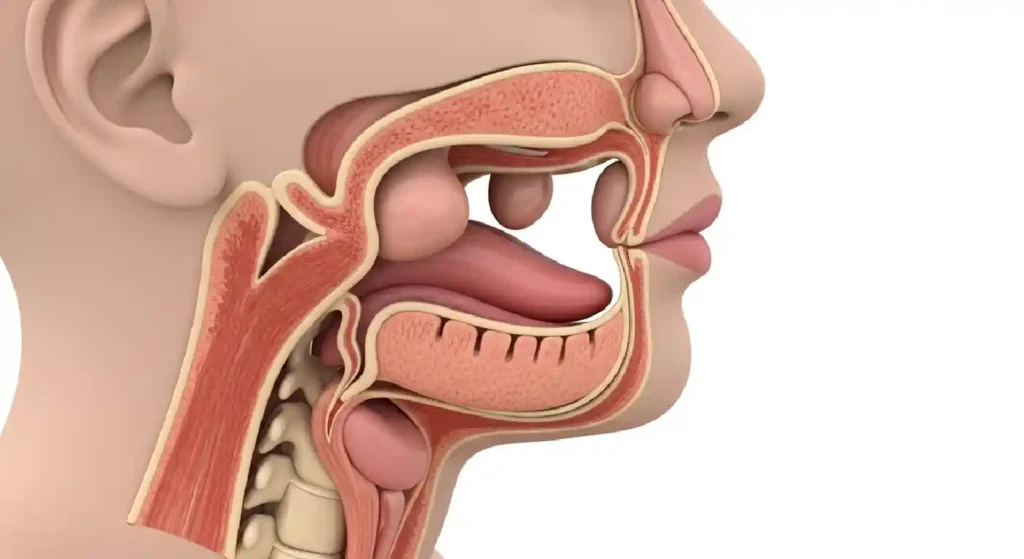
Adenoids are small lumps of tissue sitting at the back of the nasal passage, just above the throat. You can’t see them without medical equipment, but they play an early role in your immune system — especially during childhood.
Adenoid hyperplasia simply means the adenoids have grown larger than normal. In most kids, adenoids shrink naturally as they get older. But when they enlarge and stay that way, they start blocking airflow and cause a cascade of problems.
Common causes include:
- Repeated respiratory infections (colds, sinus infections)
- Chronic allergies
- Viral infections like Epstein-Barr virus
- Gastroesophageal reflux (yes, acid reflux can contribute)
- Genetic predisposition — it often runs in families
Children between ages 3 and 7 are the most commonly affected, though adults can develop it too, particularly if they have persistent allergies or immune issues.
How Do You Know If Someone Has It? Key Symptoms to Watch
The symptoms of adenoid hyperplasia are pretty hard to ignore once they escalate. The challenge is that they often mimic other conditions, so many families spend months bouncing between diagnoses before landing on the right one.
The most common signs include:
- Persistent nasal congestion that doesn’t respond to medication
- Loud snoring or noisy breathing during sleep
- Breathing through the mouth instead of the nose
- Frequent ear infections or fluid in the ears
- Muffled voice or speaking as if the nose is plugged
- Restless sleep or pauses in breathing (sleep apnea)
- Trouble concentrating or behavioural changes in children
In adults, symptoms are similar but may also include chronic sinusitis and persistent post-nasal drip.
One practical example: a seven-year-old who starts doing poorly in school, seems tired all the time, and snores heavily at night might actually be suffering from disrupted sleep caused by enlarged adenoids — not laziness or attention issues. Once treated, many parents report dramatic improvements in their child’s focus and energy.
What Does the 571 Number Mean? A Complete Guide
Diagnosis: What to Expect at the Doctor’s Office
Getting a proper diagnosis usually involves a visit to an ENT specialist (ear, nose, and throat doctor). The process isn’t complicated, but it does require the right tools.
Here’s what typically happens:
- Nasopharyngoscopy — a small, flexible camera inserted through the nostril to directly visualise the adenoids
- X-ray of the nasopharynx — a lateral neck X-ray can show adenoid size
- Sleep study — recommended if sleep apnea is suspected
- Hearing test — to assess whether fluid buildup has affected hearing
Early diagnosis matters. Children who go undiagnosed for years can develop what doctors call “adenoid facies” — a set of facial changes including an open mouth appearance, elongated face, and dental problems caused by prolonged mouth breathing.
Treatment Options for Adenoid Hyperplasia
Treatment depends on severity. Mild cases can often be managed without surgery, while more severe blockages usually require a procedure.
Non-Surgical Approaches
For mild to moderate cases, doctors often start with conservative treatment:
- Nasal corticosteroid sprays — reduce inflammation and shrink the adenoids over time
- Antihistamines — helpful if allergies are driving the enlargement
- Saline nasal rinses — keep nasal passages clear and reduce irritation
- Treating underlying infections — antibiotics if bacterial infection is confirmed
- Managing reflux — dietary changes and medication to reduce acid exposure
These options work well for many children, especially if the enlargement is mild and not causing significant breathing or sleep issues.
Surgical Treatment: Adenoidectomy
When conservative treatment fails or the symptoms are severe, an adenoidectomy (surgical removal of the adenoids) is the standard solution. It’s one of the most commonly performed surgeries in children and has a strong safety record.
The procedure is typically done under general anesthesia and takes about 30 minutes. Recovery usually involves a few days of rest, soft foods, and mild discomfort. Most children bounce back quickly and see immediate improvement in breathing and sleep quality.
In many cases, a tonsillectomy is performed at the same time if the tonsils are also enlarged.
Pros and Cons of Adenoidectomy
Understanding both sides helps families make informed decisions.
Pros:
- Rapid and lasting relief from nasal obstruction
- Significant improvement in sleep quality
- Reduces frequency of ear infections
- Can improve speech and hearing
- Short recovery time
Cons:
- Carries the standard risks of general anesthesia
- Small chance of bleeding post-surgery
- Adenoids can occasionally regrow, especially in younger children
- Not always necessary in mild cases
Common Mistakes People Make with Adenoid Hyperplasia
It’s easy to mismanage this condition, especially early on. Here are some mistakes worth avoiding.
1. Assuming it’s just allergies Many parents (and even some GPs) attribute all the symptoms to allergies and treat accordingly for months without improvement. If nasal sprays and antihistamines aren’t working after 6–8 weeks, push for a referral to an ENT.
2. Delaying treatment in children with sleep apnea Sleep-disordered breathing in children is serious. It affects brain development, behaviour, and academic performance. Don’t wait it out hoping they’ll “grow out of it” without professional guidance.
3. Skipping follow-up after surgery Surgery isn’t always the final step. Post-op care, hearing checks, and monitoring for regrowth are all part of proper management.
4. Ignoring it in adults Adults often dismiss chronic congestion as just a normal part of life. Persistent symptoms deserve proper evaluation — adenoid hyperplasia in adults, though less common, is very treatable.
5. Not addressing underlying triggers If allergies or reflux are driving the enlargement, they need to be treated too. Removing the adenoids without managing root causes can lead to recurrence or continued discomfort.
Best Practices for Managing Adenoid Hyperplasia
Whether you’re dealing with this condition yourself or helping a child through it, these practical steps make a real difference.
- Act early — the sooner you get a diagnosis, the easier treatment tends to be
- Work with a specialist — an ENT has the tools to properly visualise and assess adenoid size
- Keep a symptom diary — tracking symptoms helps your doctor understand the pattern and severity
- Don’t skip allergy management — keeping allergen exposure low reduces ongoing inflammation
- Create a good sleep environment — elevating the head slightly and using a humidifier can ease nighttime symptoms
- Educate teachers and caregivers — children with untreated adenoid issues may seem inattentive or slow; making their environment aware prevents unnecessary labels
- Follow post-surgical instructions closely — proper recovery after adenoidectomy reduces complications significantly
Conclusion
Adenoid hyperplasia is far more common than most people realise, and its impact — especially on children — can be significant. From disrupted sleep to ear infections to changes in facial development, the consequences of leaving it unmanaged stack up over time.
The good news is that this condition is well understood and very treatable. Whether through medication or surgery, most people see meaningful improvement relatively quickly. If something feels off — your child snores too much, gets too many ear infections, or never seems to breathe comfortably through their nose — trust your instincts and get it checked out. The earlier you catch it, the smoother the road ahead.
Frequently Asked Questions (FAQs)
1. Can adenoid hyperplasia go away on its own?
In some children, mild enlargement does reduce naturally as they get older and the immune system matures. However, if symptoms are affecting sleep, hearing, or quality of life, waiting it out isn’t recommended without medical guidance.
2. Is adenoid hyperplasia the same as having swollen tonsils?
No, they are different tissues. The tonsils are visible at the back of the throat, while adenoids sit higher up behind the nasal passage. They can both be enlarged at the same time, but they are separate structures.
3. How is adenoid hyperplasia treated in adults?
Adults are typically treated with nasal corticosteroids, allergy management, and treatment of any underlying infections. Surgery is an option when conservative treatments don’t provide enough relief.
4. Will my child’s speech improve after adenoid removal?
Yes, in many cases. The muffled, nasal-sounding speech caused by blocked nasal passages often improves noticeably after adenoidectomy, sometimes within just a few weeks.
5. Can adenoids grow back after surgery?
Yes, though it’s not common. Regrowth is more likely in very young children. If symptoms return after surgery, a follow-up with an ENT can determine whether regrowth has occurred.